- Blog
- Street racing syndicate widescreen fix
- Multimon security software
- Timer 2 minutes
- Bookwright image resolution
- Personal consumption expenditures
- Xnip motor spark plug wires
- Pmp cancer
- Sixtyforce rom files
- Solr suggester example
- Pixel 3 civilization beyond earth wallpapers
- Eso petrify
- Stardew valley fishing guide
- Fallout 76 mutations
- Hex file viewer
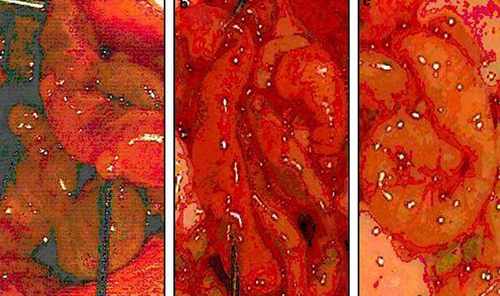

A Cox proportional hazard model was used to analyze the effect of several clinical and pathologic factors on disease-specific survival (DSS) and disease-free survival (DFS). In some patients, a second procedure was performed after recurrence or progression. The analyses were performed on patients treated for PMP between 19. PMP was classified retrospectively into 3 pathologic subtypes according to Ronnett's criteria: disseminated peritoneal adenomucinosis (DPAM), peritoneal mucinous carcinomatosis (PMCA), and an intermediate group (PMCA-I). Completeness of cytoreduction is recorded at the end of surgery: no residual macroscopic tumor (R1), residual macroscopic tumor smaller than 2.5 mm in any region (R2a), and tumor deposits larger than 2.5 mm in any region (R2b).ĭata were obtained from a prospective database of clinical records, surgical reports, reports of CT scans, laboratory and pathology reports, and contact with the patient's general practitioner. Maximum diameter of tumor deposits are graded into 0 cm, 1 to 5 cm, and >5 cm. A specialized surgical team performs the treatment.Īt surgery, tumor load is recorded in 7 distinctive abdominal regions: pelvis, ileocecum, omentum/transverse colon, small bowel/mesentery, subhepatic region, and subphrenic left and right regions. At the end of the procedure, the necessary anastomoses are made. This is followed by intraoperative HIPEC with mitomycin C 35 mg/m 2 for 90 minutes at 40☌ to 41☌ to erase microscopic residual tumor. 12 Briefly, this treatment modality consists of resecting (potentially) all macroscopic tumor deposits on parietal and/or visceral peritoneal surfaces, combined if necessary with resection of involved viscera. The principles of cytoreductive surgery and HIPEC have been described in detail elsewhere. The aim of this study is to evaluate this treatment strategy in terms of survival, and to identify clinical and pathologic prognostic factors for survival. 5Īt The Netherlands Cancer Institute, aggressive cytoreductive surgery in combination with intraoperative hyperthermic intraperitoneal chemotherapy (HIPEC) is used as the treatment of PMP since 1995. Consequently, PMP always results in the death of the patient unless radically treated. Gastrointestinal function is compromised and eventually obstruction is imminent. 9–11 As PMP progresses, the excessive mucous accumulation causes compression of the intestines. In other cases, they present with an inguinal herniated sac or an ovarian mass. Sometimes patients present themselves with symptoms arising from the primary tumor, mimicking appendicitis. It mainly expresses as a so-called “jelly belly,” caused by the abundant intraperitoneal mucous. 7,8Ĭlinically, PMP is a slowly progressive disease. 1,3–6 Incidental PMP has unusual origins. 2 PMP is reported to originate from mucinous (cyst)adenoma, mucoceles, and mucinous (cyst)adenocarcinoma of mostly appendix (or ovary). These implants are the final stage of a distribution process following the rupture of an intraperitoneal located mucinous neoplasm. 1 It is characterized by intraperitoneal disseminated mucous produced by adenomucinous tumor cells in implants on peritoneal surfaces. Pseudomyxoma peritonei (PMP) is a rare disease with an incidence of approximately 1 per million a year.
- Blog
- Street racing syndicate widescreen fix
- Multimon security software
- Timer 2 minutes
- Bookwright image resolution
- Personal consumption expenditures
- Xnip motor spark plug wires
- Pmp cancer
- Sixtyforce rom files
- Solr suggester example
- Pixel 3 civilization beyond earth wallpapers
- Eso petrify
- Stardew valley fishing guide
- Fallout 76 mutations
- Hex file viewer
